801-797-2297
1414 South 600 West, Bountiful, UT 84010
Mon-Friday, 8am-5pm
801-797-2297 | Mon-Friday, 8am-5pm
Vasolabs Is A Premier Provider Of Safe, Convenient Heart Disease Screenings.
Vasolabs Is A Premier Provider Of Safe, Convenient Heart Disease Screenings.
Uses the newest ultrasound technology
Determines whether or not you have heart disease
Pain-free. Requires no wires, treadmills, or needles.
Takes only 15 minutes
Get your Easy-to-Understand Report within 24 hours
Optional Discussion with your Clinician
Schedule a test to see if you’re at risk of heart disease!
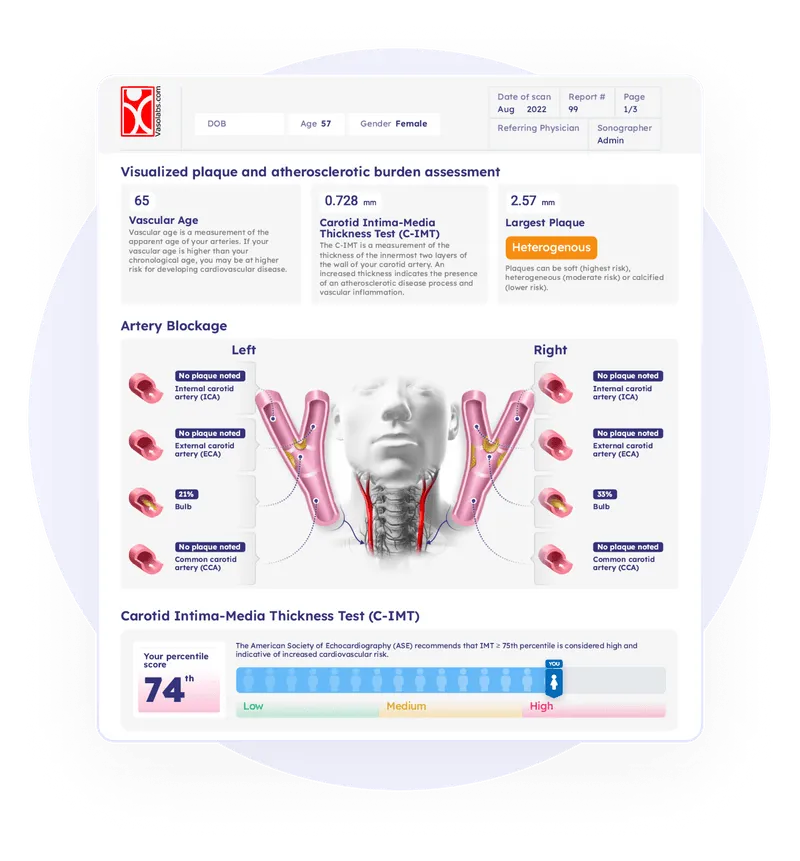
Identify Your Risks of Getting Cardiovascular Disease With a Simple C-IMT Scan!
Loved ones depend on you.
Do I Need a Heart Screening?
Here is a checklist of factors that put you at elevated risk for heart attack, stroke, and other forms of cardiovascular disease:
Over 40 years of age
Family history of heart disease/stroke
Overweight
Increased cholesterol level
High-fat diet
Tobacco user
High blood pressure
Diabetic
Metabolic syndrome
Erectile dysfunction
Psoriasis
Peace of Mind is Priceless

Looking back, it's chilling to realize how close I came to the edge. I opted for a test at Vasolabs on a whim, without any particular symptoms. Boy, am I glad I did! Turns out, my arteries were nearly clogged up - something regular doctors wouldn't have caught unless there were signs of a problem. By the time I got a couple of second opinions and returned to my regular doctor, my arteries were 95% blocked. If I hadn't taken the test when I did, I could have had a stroke. Trust me when I say this, going to Vasolabs was one of the best decisions I've ever made.
- George B

I was really worried about getting a heart attack because its already happened in our family. So taking this test gave me the peace of mind I was looking for. And it was so cool to see the age of my artery was younger than I was!!
- Barbara L.

I went to Vasolabs for their C-IMT testing, thinking it'd be a complicated deal, but nope! It was as easy as getting a photo taken. And guess what? They found an issue that could've been a silent threat. Thanks to them catching it early, my doctor and I are on top of it now. Honestly, I feel like I dodged a bullet. Big thumbs up for Vasolabs!
- Walter S.

I saw an ad on Facebook and I got the C-IMT Test for myself and my husband, it was such an easy process. And a great gift idea for family. It was really fun to look at the results and good to know I need to work on my health.
- Jessica F.
Frequently Asked Question
What is a C-IMT scan?
A C-IMT Scan is a non-invasive procedure that uses ultrasound technology to measure the thickness of your carotid arteries' walls. These arteries, located on each side of your neck, supply blood to your brain. Over time, plaque can build up in these arteries, causing them to thicken. This is often an early sign of atherosclerosis, a disease that can lead to serious conditions such as heart attacks and strokes.
Where do I go to get this scan?
For your quick, 15-minute appointment, simply head over to our facility located at 1414 South 600 West, Bountiful, UT 84010.
Who takes my test?
Dean Ence, an expert sonographer, will be handling your fast, no-pain test to figure out the 'age' of your arteries. This test checks how thick your artery walls are - thicker walls can mean inflammation. It's all simplified for you to understand easily. We also spot and show plaque, whether soft or hard, in your arteries. You get detailed pictures from the ultrasound for your records. Taking care of your health is our main goal!
How long does the C-IMT Scan and Report take?
The duration of the C-IMT scan can vary depending on various factors, like the complexity of the patient's condition. Typically, a Vasometric scan takes around 15 minutes to complete. The report is done and delivered within 24 hours to you.
Will my insurance cover this C-IMT Scan?
Most insurance providers don't cover the cost of this scan. However, most hospitals are around $800 a scan, but we are only charging $199!
Hospitals often inflate prices due to the complex nature of their billing systems and agreements with insurance companies.